
Degenerative Joint Disease of the Shoulder



The shoulder joint is formed where the humerus (the upper arm bone) meets the scapula (the shoulder blade).
The top of the humerus forms a ball known as the head of the humerus. The scapula forms a shallow cup
known as the glenoid. This forms the shoulder socket. The ball and socket joint of the shoulder is known as the
glenohumeral joint.
The surfaces of the humeral head and glenoid are capped with a layer of cartilage. The cartilage that caps the
ends of bones in joints is known as articular cartilage. Articular cartilage is smooth and slippery. This lowers
friction in the joint and allows the bones to glide smoothly against one another as the shoulder moves. Articular
cartilage is slightly softer and more rubbery than bone. A thick, viscous fluid known as synovial fluid (joint
fluid) fills the joint. Together, the articular cartilage and synovial fluid provide a cushion between the bones.
The joint is surrounded by a capsule known as the synovium which keeps the synovial fluid from leaking out.
The shoulder joint is built to allow for a wide range-of-motion. This allows the arm to reach high overhead,
out to the side, behind the back, and out in front of the body. However, because of its great mobility, the
shoulder is one of the less stable joints in the body. In other words, it dislocates more easily than other joints.
A ring of fibrous cartilage surrounds the glenoid. This is known as the labrum. The labrum helps to fit the
shallow glenoid to the round head of the humerus. This deepens the socket and helps to make the shoulder
more stable.
Ligaments (fibrous structures that hold one bone to another bone) and tendons (fibrous structures that hold
muscles to bones) help to stabilize the shoulder as well by holding the humeral head in the socket. Among these
tendons is the rotator cuff. The rotator cuff is a group of muscles that act to rotate and elevate the arm. Their
tendons surround and attach to the humeral head, forming a cuff. Together, they pull the humeral head into the
glenoid and help to keep it from dislocating.
Degeneration of the Shoulder Joint
The blood supply to articular cartilage is poor. Without a healthy blood supply, nutrients are not readily
available to the cartilage tissue. When it is damaged, it does not heal as well as bone, skin, muscle, or other
tissues.
Years and decades of use can take their toll on the articular cartilage in any joint. The shoulder is no exception.
As the glenoid and humeral head rub and strike against one another, the cartilage can begin to soften and crack.
Because cartilage does not heal as well as other tissue, the damage to the cartilage tends to worsen. Over time
cartilage can peel away, exposing bare bone. As the smooth cushion between the humeral head and glenoid
erodes, the bones begin to grind against one another. This causes pain, grinding, and stiffness. The condition
has several names including degenerative joint disease, osteoarthritis, or simply arthritis.
Everyone is subject to the wear and tear of arthritis. In theory, everyone who lives long enough will end up with
arthritis in the shoulders. Why one person develops shoulder arthritis at a younger age than another person can
be a difficult question to answer. Factors include genetics, lifestyle, injuries, and other medical problems.
Arthritis that results from a specific injury or disease process is called secondary arthritis. Arthritis with no
readily identifiable cause is known as primary arthritis.
A traumatic injury to the shoulder can instantly damage the articular cartilage and speed up the process of
degeneration. For example, a blow to the shoulder may fracture the glenoid and crack the articular cartilage.
Once the cartilage has cracked, it is easier for it to peel away. Think about removing the shell from a hard-boiled
egg. It is impossible to simply peel off the shell. But once the shell is cracked it is easy to remove the cracked
pieces. Arthritis that results from a traumatic injury is known as post-traumatic arthritis.
Other medical problems such as gout, infection, and rheumatoid disease can be very hard on the joint and
speed up the degenerative process.
Many people who develop shoulder arthritis state that they have a parent, sibling, or grandparent who also
suffered with arthritis. "It runs in the family," they claim. There is likely a genetic component that plays a
role in the development of arthritis at a younger age.
Shoulder instability can also speed up the degenerative process. If the humeral head does not sit securely in
the glenoid, it changes the mechanics between the two bones. This may place more pressure on one area of the
humeral head or glenoid, causing the cartilage in that area to wear away more quickly. Several structures are
involved in shoulder stability including the labrum, rotator cuff, glenoid, joint capsule, shoulder ligaments, etc.
Dysfunction of any of these structures can affect the mechanics of the shoulder. This dysfunction may be subtle
and might not be identified.
A lifestyle that involves heavy labor or repetitive shoulder activity can contribute as well. If the wear and tear
placed on the articular cartilage exceeds its ability to heal, the cartilage will begin to degenerate.
Most people who develop osteoarthritis of the shoulder are unable to identify a clear cause.
The severity of shoulder arthritis is often described using the term "chondromalacia." Chondromalacia
means "softening of the cartilage." Grade I chondromalacia is when the cartilage begins to soften. Grade II
chondromalacia is when the cartilage begins to crack and fissure. The cartilage begins to look like crab meat at
grade III. Grade IV chondromalacia is when the cartilage has completely worn away, exposing bare bone. The
entire surface of the bone does not wear away at the same speed. One area of the humeral head may have grade
II chondromalacia while another area has grade IV chondromalacia.
Diagnosing Shoulder Arthritis
History
People with osteoarthritis of the shoulder complain of pain within the shoulder joint. They may complain of
pain with attempting to use the arm, especially with overhead activity. Often, they complain of a grinding or
popping sensation within the shoulder joint as they move the arm. This is known as crepitus. The onset of pain
is usually gradual, and pain worsens over a period of months to years.
Occasionally, arthritic pain begins after an injury. A person may fall or otherwise injure the shoulder. They seek
medical treatment expecting to have a fracture, sprain, or other injury. They are surprised to find out that they
have arthritis (and that they had had arthritis since before the injury). Some people function well and have
minimal pain with shoulder arthritis. An injury can aggravate the arthritic shoulder, resulting in a dramatic
increase in shoulder pain.
ྕ
Pain with shoulder movement
ྕ
Gradual onset of worsening shoulder pain
ྕ
Grinding or popping
Physical Exam
A thorough physical examination seeks not only to find evidence of osteoarthritis, but also to rule out other
causes of shoulder pain such as fractures, biceps tendinitis, rotator cuff tears, labral tears, nerve damage, etc.
The shoulder usually appears essentially normal. The shoulder may be tender around the deltoid and
glenohumeral joint. There may be weakness and pain with attempts to raise or rotate the arm. Popping and
grinding can sometimes be felt or even heard with shoulder movement. Just because the shoulder is arthritic
does not mean that other problems are not present as well. It is common to have both shoulder arthritis and a
torn rotator cuff.
Passive range-of-motion (the person with shoulder pain relaxes while the examiner raises the arm for them)
may be limited, depending on the severity of the degenerative changes. Normal range-of-motion:
o
Forward flexion ≈ 180°
o
Abduction ≈ 180°
o
External rotation ≈ 100°
o
Internal rotation ≈ 90°
Active range-of-motion (the person with shoulder pain attempts to raise and rotate their own arm) elicits
pain if the rotator cuff is injured or damaged.
Crepitus: Popping and grinding can be felt by the examiner as the shoulder is manipulated.
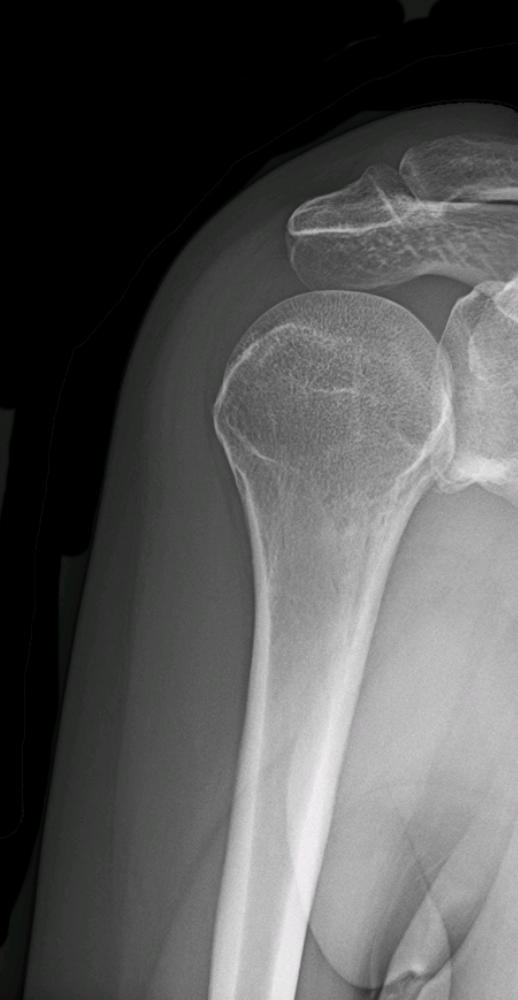
X-rays
Depending on the severity of the degenerative changes, osteoarthritis can often be readily identified on x-rays.
X-rays will demonstrate narrowing of the joint space between the humeral head and glenoid. They may also
demonstrate osteophytes (bone spurs) and sclerotic bone (bone that appears more white on x-rays because it has
hardened).
If the humeral head appears to be sitting too high in relation to the glenoid, the rotator cuff is likely torn.
X-rays are also helpful to rule out fractures, calcific tendinitis, acromioclavicular arthritis, tumors, and other
problems.
MRI (magnetic resonance imaging)
X-rays are usually sufficient for diagnosing osteoarthritis of the shoulder, especially if the arthritis is moderate
or severe. However, MRIs can be helpful in identifying early arthritic changes that are not visible on x-rays. An
MRI may also be obtained if another cause of shoulder pain is suspected such as a rotator cuff tear.
Shoulder Arthroscopy
Mild, early degenerative changes may not be visible on x-rays or even an MRI. If no definitive cause of shoulder
pain is identified and nonsurgical treatment is not effective, a diagnostic shoulder arthroscopy may be
performed. This involves introducing a slender camera called an arthroscope into the shoulder joint. The inside
of the shoulder joint can then be viewed on a monitor. During the shoulder scope procedure, the articular
cartilage is examined. A small, metal probe can be used to examine the cartilage as well.
Treating Shoulder Arthritis
Initial treatment for osteoarthritis of the shoulder is usually non-operative. Anti-inflammatory medications
(NSAIDs) such as ibuprofen may help to reduce pain and inflammation. A steroid (cortisone) injection into the
glenohumeral joint may also be very helpful. Physical therapy can help with stretching, range-of-motion
exercises, strengthening, and scapular stabilization.
NSAIDs
Intra-articular (into the joint) steroid injection
Rest (avoid strenuous, repetitive activity with the shoulder)
Ice
Physical therapy
If symptoms do not improve with more conservative treatment, surgery may be recommended.
Surgical options for shoulder arthritis include:
Arthroscopic debridement: During a shoulder scope, the damaged cartilage may be smoothed and
trimmed. This may provide temporary relief from arthritic shoulder pain, but is not a definitive treatment.
This surgery may be considered if:
o
Arthritic changes are mild
or
o
Shoulder arthroscopy is being considered to address other causes of shoulder pain in addition to
the arthritis
or
o
Shoulder replacement is not an option
Resurfacing hemiarthroplasty: The head of the humerus is partially removed and replaced with a
metal implant. If arthritic changes involve both the humeral head and glenoid, this is probably not a good
option. This surgery may be considered if:
o
Arthritic changes are present only on the humeral head and not the glenoid
and
o
There is a desire not to remove too much bone
Hemiarthroplasty: The head of the humerus is removed and replaced with a metal prosthesis that has a
stem that implants in the shaft of the humerus. This is commonly used to treat fractures of the humeral
head and neck. If the glenoid is arthritic as well, this is probably not the best option. This surgery may be
considered if:
o
Arthritic changes are present only on the humeral head and not the glenoid
or
o
The glenoid does not appear capable of holding a glenoid prosthesis
Total shoulder arthroplasty: The head of the humerus is removed and replaced with a metal prosthesis
that has a stem that implants in the shaft of the humerus. The glenoid is also replaced with a prosthesis.
This is a traditional shoulder replacement. It provides great pain relief. However, if there is a large rotator
cuff tear it may not be the best option. This surgery may be considered if:
o
Degenerative changes are severe
and
o
The rotator cuff is intact
Reverse total shoulder arthroplasty: Reverse total shoulder replacement is similar to a traditional
shoulder replacement. However, the head of the humerus is replaced with a concave implant (cup) and
the glenoid is replaced with a convex implant (ball). In other words, the ball becomes the socket and the
socket becomes the ball. This changes the mechanics so that an intact rotator cuff is not necessary. This
surgery may be considered if:
o
Degenerative changes are severe
and
o
There is a large rotator cuff tear
or
o
A previous shoulder replacement was done and failed
The traditional surgery for osteoarthritis of the shoulder is called total shoulder arthroplasty (shoulder
replacement).
Shoulder replacement surgery is usually done under general anesthesia (completely asleep). An injection may
also be given by the anesthesiologist to numb the shoulder and arm.
An incision is made over the front of the shoulder. Soft tissue is dissected out of the way and the shoulder joint
is exposed. The humeral head is dislocated and removed. The glenoid is reamed and prepared to receive a
prosthetic cup. A prosthetic humeral head is then implanted into the shaft of the humerus. The humerus, with
its new humeral head, is pushed back into place in the shoulder socket. The soft tissue around the joint is
repaired and the skin is closed. The incision is then dressed and the arm is placed into a sling.
Not everyone with severe shoulder arthritis is a good candidate for surgery. A shoulder replacement is an
elective surgery and, while relatively safe, is not risk free. The heart, kidneys, and other organs must be healthy
enough for anesthesia. People with infections such as tooth abscesses, urinary tract infections, and skin sores
should not undergo shoulder surgery because of the risk that the infection may spread to the shoulder joint.
People with poorly controlled diabetes are poor surgical candidates because of the risk of infection and poor
wound healing.
If a rotator cuff tear is present, a traditional total shoulder replacement may not be a good option. Shoulder pain
may persist even after surgery because of the torn rotator cuff. This also makes it difficult to raise the arm out to
the side. In a reverse total shoulder replacement the ball and socket are switched. By switching the ball and
socket, the mechanics of the shoulder are changed so that the deltoid muscle can take over for the rotator cuff in
raising the arm to the side.
Whether a traditional total shoulder replacement or a reverse total shoulder replacement is performed, a short
hospital stay is usually advised. Pain medication is made available and ice is applied to the shoulder. Physical
therapy begins the day after surgery. Medication and other precautions are often recommended to lower the risk
of developing a blood clot following surgery. No active use of the arm or shoulder is permitted.
Rehabilitation Following a Shoulder Replacement
For the first four to six weeks, the goal is to allow the soft tissue to heal, protect the prosthesis, and restore some
passive range-of-motion of the shoulder. If there is too much activity following surgery, healing may be delayed
and damage may be done to the prosthesis. If there is not enough movement following surgery the shoulder may
become stiff.
Gentle passive range-of-motion exercises are begun. In other words, the muscles of the shoulder should not be
used to raise or rotate the arm, but the arm can be moved gently by a physical therapist. The sling is worn for
the first few weeks.
After the first four to six weeks, more aggressive stretching can begin. Assisted active range-of-motion may
begin as well. This means that the shoulder muscles can be used to begin raising the arm, but only with the
assistance of a physical therapist, a well-instructed family member, or other trained person.
After several weeks, as the repair continues to heal, the surgeon and physical therapist will determine that it is
time to begin active range-of-motion. As passive and active range-of-motion improve, strengthening exercises
may begin later on.
Full recovery following a shoulder replacement takes about four to 6 months.
Expectations Following a Shoulder Replacement
Immediately following surgery, arthritic pain will be replaced with postoperative pain. Pain will gradually
improve. Most people are very glad that they had the shoulder replaced after six to eight weeks.
Shoulder replacement surgery is helpful in reducing pain and improving function. However, range-of-motion
will not return to the level it was before shoulder problems began. Most surgeons recommend against strenuous
activity such as heavy manual labor following a shoulder replacement.
The implanted prosthesis does not last forever. A total shoulder prosthesis is said to last about 15 years, but this
varies greatly from person to person and is impossible to predict.




















