
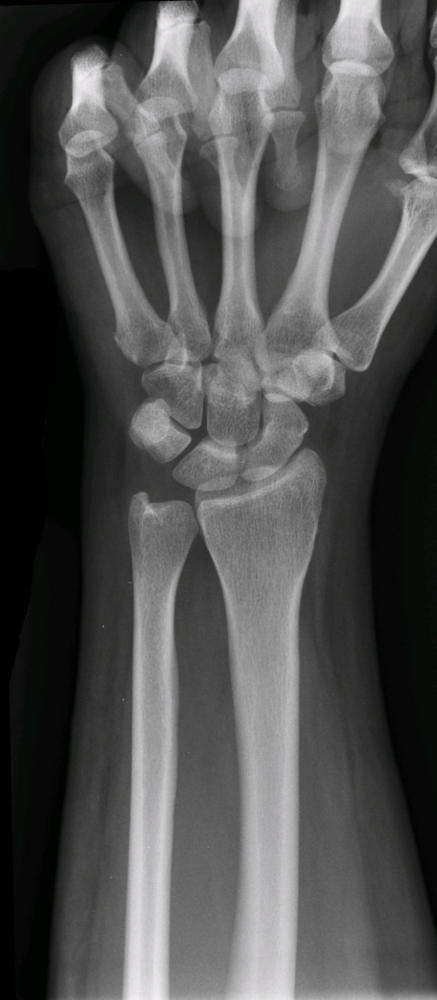
Metacarpal Fracture






Fractures at the base of the 1st metacarpal involve the carpometacarpal, or CMC, joint of the thumb. This joint is
very important in gripping and pinching. A fracture through the base of the metacarpal can damage the joint,
causing it to degenerate and become arthritic. This is known as post-traumatic arthritis. Two specific fracture
patterns have been named. Bennett's fracture involves the ulnar side of the metacarpal base. Rolando's fracture is a
"Y" or "T" shaped fracture of the metacarpal base that may be very comminuted, meaning that it is broken into many
pieces.
The CMC joint of the thumb has been described as two interlocking saddles. This allows for movement in 2
planes. Among the tendons that attach to the 1st metacarpal are the abductor pollucis longus and the adductor
pollucis. A Bennett's fracture may occur when a violent axial force is applied to the thumb in a slightly flexed
position. The abductor pollucis longus has a tendency to pull the metacarpal down and out while the adductor
pollucis pulls the head of the metacarpal in. This results in slight dislocation (also known as subluxation) and
displacement at the fracture site.
Even fractures that initially appear nondisplaced may displace over time because of the tension applied by these
tendons. If the fracture is allowed to heal in this position, it can change the mechanics of the thumb and lead to
arthritic changes. The end result is a weak grip, poor range of motion, and chronic pain.
Bennett's fractures are usually treated surgically. The fracture can be pulled back into alignment either my
making an incision and looking right at the bone or closed underneath a fluoroscope (which is like a small x-ray
machine.) Pins or screws are then used to hold the fragments in place. Several different methods of placing the pins
or screws are available depending on the nature of the fracture.
Rolando's fractures have a worse prognosis, especially if they are very comminuted. If there is a simple "T" or
"Y" fracture, open reduction and internal fixation is a good option. An incision is made over the fracture site. The
fracture is reduced, or pulled back into alignment. A pin is used to hold the fragments in place along with reduction
forceps. A T-shaped plate is then applied and the pin removed.
If the fracture is very comminuted, open reduction and internal fixation will likely not lead to a good outcome.
Instead, pins or an external fixator can be used to hold the metacarpal in place, allowing the many fragments to heal.
Even with appropriate treatment, Rolando's fractures may result in post-traumatic arthritis and chronic pain. If so,
the CMC joint can be fused. This will eliminate the pain caused by the arthritic joint, but will result in limited range
of motion.
The long bones of the hand are called the metacarpals. There are 5 metacarpals -- one for each finger. An injury to
the hand can break one or more of the metacarpals. This is known as a metacarpal fracture.
Metacarpal fractures usually result from a traumatic blow to the hand. Metacarpal fractures may involve the head,
neck, shaft, or base of the metacarpal. Fractures of the 5th metacarpal neck are especially common. They typically
occur with punching a hard object and are known as boxer fractures.
Metacarpal fractures are diagnosed based on a history, physical exam, and x-rays. Patients may report punching a
wall or another traumatic blow to the hand.
Upon physical exam, the hand may be bruised and swollen. The broken bone will, of course, be tender to push on.
There may be a deformity at the fracture site. The knuckle associated with the broken metacarpal may be less
prominent. The fingers are inspected to look for rotational deformities.
X-rays are important not only to confirm that the hand is broken, but to evaluate the fracture. Fractures may be
non-displaced (just a crack) or displaced. They may involve the cartilage in the joints (intra-articular). They may be
angulated (bent at the fracture site).
Non-displaced metacarpal fractures can be treated without surgery. A cast or splint is applied to immobilize the
affected fingers and limit motion across the fracture site. This prevents the broken fragment from displacing
(moving out of place) and allows the fracture to heal. The fracture takes 4 to 6 weeks to heal.
If the metacarpal fracture is displaced or angulated, it must be reduced. This means that the fracture is pushed back
into alignment. If a stable reduction can be obtained, a cast or splint is applied to hold the fragments in place and
allow the fracture to heal.
If the fracture is too displaced or unstable, especially if it involves the joint surface, an adequate reduction may not
be possible to maintain without surgery. Surgery sometimes involves pushing the fracture fragments back into place
and then drilling a pin through the skin and across the fracture site to hold the fragments in position. This is known
as percutaneous pinning or closed reduction-internal fixation (CRIF). Pins are usually removed in the office in 3 to
5 weeks.
Occasionally, the fracture cannot be successfully reduced without making an incision and exposing the bone. This is
known as open reduction-internal fixation (ORIF). Screws or plates may be used to fix the fragments in place.
These are generally not removed.







